Ever looked at your aging report and wondered how seemingly clean claims the ones that passed your internal edits and left your team feeling confident quietly turned into long-standing accounts receivable?
Your team followed the process.
Claims were accurate.
No immediate denials.
And yet weeks passed… and the payment still didn’t arrive.
By the time someone noticed, the account had already slipped into a higher aging bucket, making recovery harder, requiring escalations, rework, and more staff time. This isn’t just inefficiency, it’s a cost center disguised as normalcy.
These situations aren’t rare outliers. They unfold quietly every day across independent practices, specialty groups, and even major hospital revenue cycle departments.
Traditional AR workflows rely heavily on static worklists, manual tracking, and human vigilance systems designed for predictable times but struggling to manage today’s complex payer behaviors. The result isn’t always a dramatic denial. More often, it’s delay. And over time, delay becomes revenue leakage.
As payer rules grow more complex and timelines more variable, the margin for timing errors keeps shrinking. By 2026, intelligent AR monitoring isn’t just a “nice-to-have” tool, it’s becoming a financial necessity.
This blog walks you through:
- Why missed follow-ups are one of the most expensive blind spots in AR
- How AR Notification AI Agents change the recovery equation
- The measurable impact on cash flow, staff efficiency, and AR stability
- Real-world scenarios where early signals prevent revenue loss
- How Claimity.ai helps revenue teams modernize follow-up intelligence
The Revenue Problem That Rarely Gets Diagnosed Correctly
Most healthcare finance discussions orbit familiar KPIs: denial rates, net collection percentages, days in AR. While these metrics matter, they often describe outcomes after the fact, rather than revealing why deterioration began.
Industry benchmarks illuminate how subtle follow-up delays translate into real financial pressure:
- The average days in AR for physician practices climbed to 61 days in 2023, up from 45 days in 2019. This extended timeline is due in part to interoperability and workflow challenges.
- Across the system, U.S. hospitals lose an estimated $150 billion annually due to claim denials, with 40% of those denials considered preventable.
- Denial rates are creeping upward, initial denial percentages have been reported around 11.8–12%, up year over year.
- Industry targets suggest that a healthy denial rate should be <5% and Days in AR under 30–40 days; anything above these thresholds usually signals significant revenue risk.
These numbers paint a consistent picture: delays, particularly delayed follow-ups are a core driver of financial stress in revenue cycles that appear operationally intact.
Why Missed Follow-Ups Behave Like Financial Multipliers
At first glance, a delayed follow-up seems simple a missed phone call, a report overlooked, a claim sitting in a queue. But in AR, timing is money.
When intervention is delayed:
- Recovery probability declines
- Additional documentation requests appear
- Appeals windows tighten
- Resolution effort increases
This happens because aging AR shifts the context of a claim, not just its status. Once a claim moves from 30 to 60 days, the rules, effort requirements, and payer responses begin to behave differently.
Rather than progressing linearly, the costs escalate:
A follow-up that might have taken one hour at 15 days can take ten hours at 45 days including research, payer calls, appeals, and resubmissions.
Multiply this effect across thousands of claims, and the hidden cost becomes significant.
The Executive Blind Spot: AR as a Lagging Indicator
Many organizations treat AR KPIs as outcome metrics dashboards to review performance.
But Days in AR and denial percentages are lagging indicators. They tell you what happened, but not what’s emerging.
By the time AR > 90 days becomes visible, a significant amount of financial exposure has already materialized. Industry best practices recommend keeping AR > 90 days under 15–20% of total receivables; anything higher is a red flag for cash flow instability.
Too often, leadership responds by:
- Adding headcount
- Tightening quotas
- Increasing biller throughput targets
These adjustments raise activity but do little to improve timing precision which is where revenue loss actually begins.
The problem is not effort.
It’s visibility early in the claim lifecycle.
The Structural Constraints Embedded in Traditional AR Workflows
Traditional AR workflows assume:
- Static worklists are sufficient
- Human prioritization reflects financial urgency
- Manual tracking will catch all critical risks
None of these assumptions hold in contemporary revenue cycle environments.
A claim has dozens of micro-deadlines: payment windows, appeal deadlines, documentation follow-ups, eligibility clarifications, prior authorization confirmations. Without real-time observation, many of these deadlines pass silently.
Manual tracking tools spreadsheets, calendar ticklers, work queues are inherently episodic, not continuous. They depend on staff checking in periodically, but payer systems operate 24/7. Claims don’t wait for business hours.
This mismatch means that silent delays accumulate, and by the time they register in traditional AR reports, they have already shaped financial outcomes.
Viewed systemically, traditional follow-up models expose structural gaps that directly shape revenue outcomes.
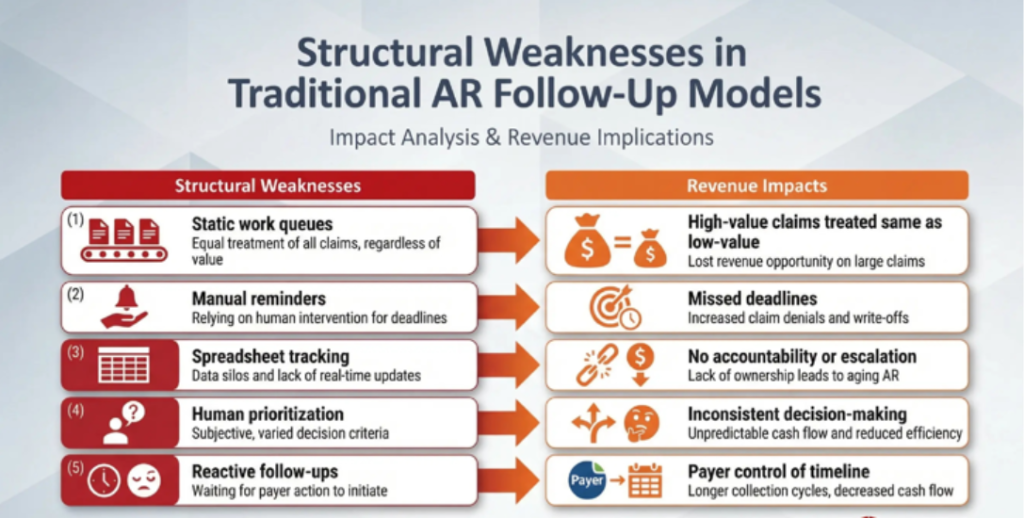
Why Human Vigilance Alone Cannot Solve Timing Variability
Humans naturally manage tasks sequentially. But claims evolve continuously. A modern healthcare provider may have tens of thousands of active claims across payers, each governed by distinct timelines, documentation requirements, and response patterns. Expecting teams to consistently detect subtle deviations in this volume is not just difficult it is structurally impossible without systemic support.
In fact:
- Around 60% of provider organizations cite manual data entry as the primary cause of revenue cycle errors, and 25% of claims require rework due to avoidable issues.
This reveals an important truth: AR challenges are rarely caused by individual mistakes. They occur because workflows were never designed to scale detailed timing awareness across changing payer behaviors.
Reframing the Problem: From Claim Tracking to Risk Tracking
Traditional AR focuses on claim status:
- Paid vs Unpaid
- Denied vs Processed
- Aging category
But status is a result, not a risk indicator.
Risk often appears long before an outcome changes. A claim that won’t respond for 20 days is more likely to slip into aging problems than one that progresses quickly. Predictive signals unusual delays, silent payer behavior, approaching deadlines are often hidden in claim metadata and patterns.
By shifting from tracking outcomes to tracking risk trajectories, organizations can intervene before the financial picture deteriorates.
This conceptual shift is the foundation of intelligent AR monitoring.
Enter AR Notification AI Agents
AR Notification AI Agents are designed to address precisely this structural gap.
Unlike passive reporting systems, these AI-augmented platforms continuously evaluate claim behavior relative to expected performance patterns and payer histories. They surface deviations not after issues emerge, but as they begin.
This means that instead of reacting to aging AR or denials, revenue teams can intervene hours or days earlier at the risk signal stage.
This isn’t just automation.
It’s proactive risk surveillance.
How AI Detects What Traditional Systems Miss
Traditional workflows wait for events:
- A denial arrives
- A payment is delayed
- A report flags an aging bucket
AI systems monitor continuously, comparing real-time claim progress against historical expectations and payer norms. When claims deviate from expected timelines even in the absence of explicit denials the system alerts teams to investigate.
This early visibility reduces the “silent lag” that often turns manageable issues into time-intensive escalations.
AI can detect:
- Claims that have stalled relative to expected trajectory
- Patterns of payer response delay
- Approaching deadline windows without corresponding activity
These patterns are difficult for humans to identify consistently at scale especially when thousands of claim threads evolve simultaneously.
Financial Prioritization Without Human Bias
Traditional prioritization often emphasizes claim balance size or age bucket. While these help categorize work, they do not capture true financial risk.
For example, a $500 claim nearing a filing limit may carry greater urgency than a $10,000 claim that’s progressing smoothly. Human prioritization even when experienced inherently introduces variability and subjectivity.
AI prioritization incorporates multiple real-time variables:
- Timing sensitivity
- Historical behavior of specific payers
- Likelihood of successful recovery
- Deadline proximity
This produces workflows aligned with financial consequence, not arbitrary administrative categories.
Why AI Strengthens Rather Than Disrupts AR Teams
There’s a common misconception that AI replaces human expertise.
In reality, AI augments it.
By removing the cognitive burden of continuous monitoring and pattern detection, AI frees staff to focus on higher-value work: resolving complex denials, handling documentation disputes, negotiating with payers, and improving front-end accuracy.
This isn’t workforce reduction.
It’s workload optimization.
The Economics of Earlier Intervention
The financial advantage of earlier intervention is not theoretical.
Evidence shows:
- Automated monitoring and proactive claim handling are associated with measurable reductions in AR days and denial rework costs. Practices that adopt automated denial management and payer tracking technologies have reported significant improvements in AR velocity and cash flow.
Claims addressed earlier consistently require fewer escalations, less rework, and exhibit greater cash predictability. When intervention moves from reactive to proactive, staff time translates into higher financial impact rather than repetitive catch-up work.
Conclusion: Revenue Stability Is an Engineering Problem
Accounts receivable deterioration is rarely the result of random events or isolated errors. It arises from structural timing variability delays that emerge quietly, accumulate predictably, and gradually erode financial performance.
Traditional models based on periodic review, static workflows, and human vigilance are not designed for today’s complex, fast-moving payer environments. These constraints create silent blind spots that translate into aging AR, increased labor costs, and reduced liquidity.
To break this cycle, organizations must adopt operational models built around continuous monitoring, earlier signal detection, and adaptive prioritization. That shift moves AR management from reactive recovery toward preventive stability and that is where sustainable revenue performance is built.
Where Claimity.ai Fits In
Modern revenue cycle strategies increasingly recognize that visibility and timing intelligence are as critical as staffing capacity. Platforms such as Claimity.ai are designed to address these structural constraints by enhancing how organizations monitor, validate, and respond to claim lifecycle events.
Claimity.ai supports revenue teams with:
- Continuous claim tracking and status visibility
- Real-time alerts for claims requiring attention
- AI-assisted validation to reduce preventable errors
- Predictive insights that help teams prioritize work effectively
- Integrated analytics that provide clearer operational signals
These capabilities don’t replace human expertise they enhance decision timing, reduce delayed detection, and help teams focus attention where financial risk or recovery opportunity is highest.
Because sustainable revenue performance is not simply about working claims faster.
It is about identifying risk sooner, responding earlier, and preventing deterioration before it compounds into denials, escalations, or long-aging AR.
FAQs
An AI system that continuously monitors claim timelines, detects deviations from expected behavior, and alerts revenue teams to emerging risks before financial deterioration becomes visible.
By detecting patterns and timing signals that traditional periodic reviews miss, enabling earlier intervention and reducing silent aging.
No. It augments staff by providing real-time risk signals so human expertise focuses where it adds the most value.
Yes, by reducing AR days, enhancing prioritization, and enabling earlier corrective action, AI contributes to more predictable and stable cash flow.